Imagine breathing in a cloud of invisible dust every day for years. You don't cough immediately. You don't feel sick right away. But deep inside your lungs, tiny particles are settling into your tissue, causing permanent scarring that you can never undo. This is the reality for millions of workers exposed to silica dust or asbestos fibers. These aren't just historical problems from old mines or demolished buildings. They are active, modern-day threats that cause thousands of preventable deaths every year.
Occupational lung diseases like silicosis and asbestosis are entirely preventable. Yet, they remain one of the most significant public health concerns in industries ranging from construction to manufacturing. The American Lung Association states clearly that these conditions should be eliminated through proper workplace interventions. If you work with stone, sand, insulation, or older building materials, understanding how these diseases develop-and more importantly, how to stop them-is not just good practice; it’s a matter of life and death.
Understanding Silicosis: The Sand That Scars
Silicosis is a chronic lung disease caused by inhaling crystalline silica dust. When you cut, grind, drill, or sand materials containing silica-like concrete, brick, stone, or sand-the process releases microscopic particles into the air. Your lungs try to trap these particles, but instead of breaking them down, your body walls them off. Over time, this creates nodules and scar tissue that stiffen your lungs, making it harder to breathe.
The history of silicosis goes back centuries. Ancient stone workers likely suffered from it, but it wasn’t until 1870 that Dr. Achille Visconti formally described "miner's phthisis" in Italian literature. Today, the data is stark. According to NIOSH data from 2018, silicosis accounts for approximately 1,200 annual deaths in the United States alone. It doesn't discriminate based on job title; it affects masons, miners, foundry workers, and even dental lab technicians who work with quartz-containing materials.
The scary part? There is no cure. Once the scarring happens, it stays. Early detection through regular spirometry testing can help slow progression, but the damage is irreversible. That’s why prevention isn't optional-it's the only strategy that works.
Asbestosis: The Fiber That Lingers
While silicosis comes from dust, asbestosis is caused by inhaling asbestos fibers. Asbestos was once hailed as a miracle material because it’s fire-resistant, durable, and cheap. It was used in everything from pipe insulation to floor tiles and roofing shingles. But when those materials are disturbed during renovation or demolition, they release fibers so small you can’t see them.
In 1906, Dr. H. Montague Murray performed an autopsy on a 33-year-old asbestos factory worker in London and identified the link between asbestos exposure and lung scarring. We’ve known about this danger for over a century. Despite bans and regulations in many countries, asbestos remains in millions of buildings. The EPA estimates that 733,000 public buildings in the US still contain asbestos-containing materials.
Between 2004 and 2014, the CDC reported 1,163 US worker deaths from asbestosis. Like silicosis, there is no safe level of exposure. The International Agency for Research on Cancer (IARC) classifies asbestos as a Group 1 carcinogen, meaning it causes cancer in humans. Even brief exposure can lead to mesothelioma, lung cancer, or asbestosis decades later.
| Feature | Silicosis | Asbestosis |
|---|---|---|
| Cause | Inhalation of crystalline silica dust | Inhalation of asbestos fibers |
| Common Sources | Concrete, stone, sand, brick | Insulation, flooring, roofing, pipes |
| Latency Period | 10-20 years after exposure | 20-40 years after exposure |
| Key Symptom | Dry cough, shortness of breath | Persistent cough, chest tightness |
| Prevention Focus | Wet cutting, ventilation, respirators | Fiber containment, abatement, PPE |
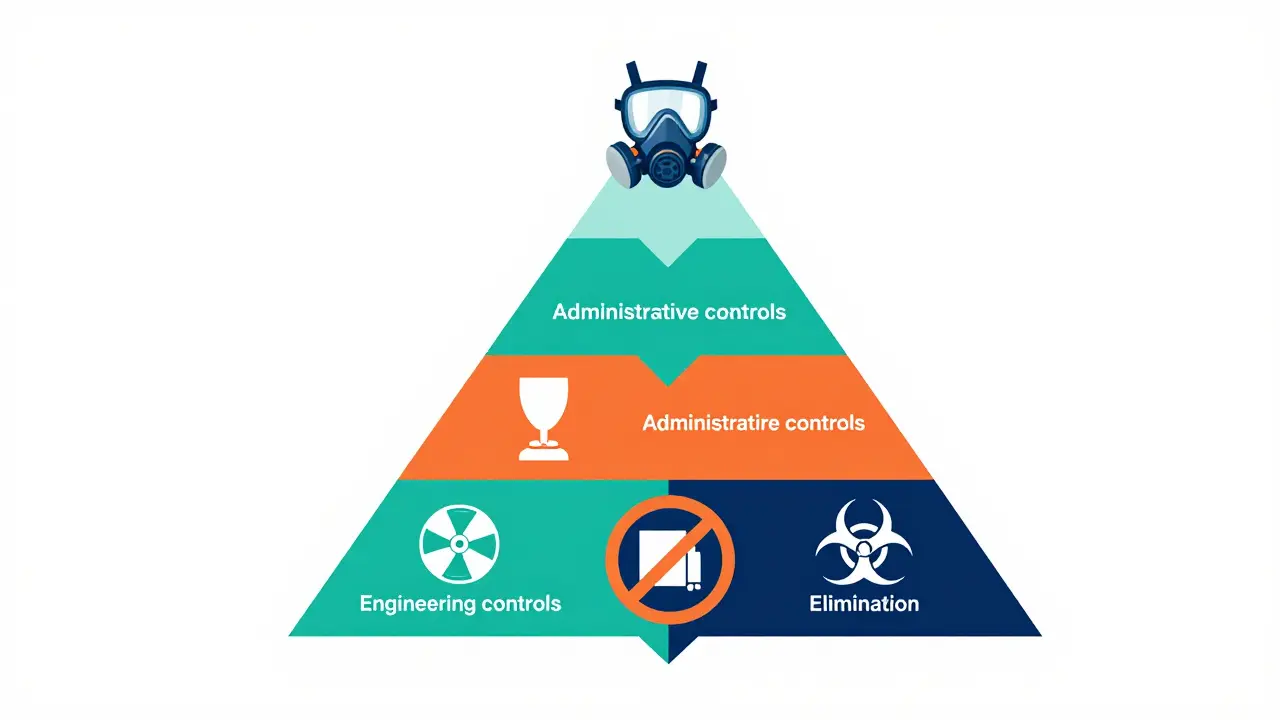
The Hierarchy of Controls: What Actually Works
You might think wearing a mask is enough. It’s not. Personal Protective Equipment (PPE) is the last line of defense, not the first. To truly protect workers, we need to follow the hierarchy of controls-a proven framework that prioritizes the most effective methods first.
- Elimination: Remove the hazard entirely. Can you substitute a non-silica material? Can you remove asbestos before starting work?
- Substitution: Replace hazardous materials with safer alternatives. For example, using fiberglass insulation instead of asbestos.
- Engineering Controls: Isolate people from the hazard. This includes local exhaust ventilation systems that capture dust at the source. OSHA standard 1910.94 recommends maintaining air velocity of 100-150 feet per minute at the contamination source to effectively capture airborne particles.
- Administrative Controls: Change how people work. Limit exposure time, rotate tasks, and post warning signs.
- PPE: Use respirators when other controls aren’t enough. But remember, PPE only works if it fits properly and is worn consistently.
According to CDC NIOSH data, engineering controls provide 80-90% exposure reduction when properly implemented. Administrative controls offer 50-70%, while PPE provides only 40-60% reduction-and that’s assuming perfect use, which rarely happens in real-world conditions.

Practical Prevention Strategies for High-Risk Jobs
If you’re working in construction, mining, or manufacturing, here’s what you need to know to stay safe.
For Silica Dust Exposure
- Use wet cutting methods. Adding water to cutting tools reduces silica dust exposure by up to 90% compared to dry cutting. Yes, it takes longer. Yes, some foremen complain. But your lungs are worth it.
- Install local exhaust ventilation. Hand tools equipped with HEPA-filtered vacuum attachments can reduce exposure by 70-80%. Make sure these systems are maintained regularly.
- Seal off work areas. Enclose operations to contain at least 95% of generated dust, as recommended by NIOSH guidelines from 2020.
For Asbestos Exposure
- Never disturb suspect materials without testing. Assume any material installed before 1980 contains asbestos unless proven otherwise.
- Hire certified abatement professionals. DIY removal is dangerous and often illegal. Proper abatement requires specialized training, equipment, and disposal protocols.
- Use P-100 respirators. Unlike N-95 masks, P-100 respirators filter out 99.97% of particles, including asbestos fibers. And yes, you need annual fit testing under OSHA standard 1910.134.
The Human Factor: Why Compliance Fails
Technology exists. Regulations exist. So why do cases still happen? Because human behavior is unpredictable. A Reddit thread from r/Construction revealed a common frustration: “My company finally got wet cutting saws last year and silica dust is way down, but the foreman still yells at us for taking too long with water methods.”
Another user shared: “I've been in demolition for 15 years and never had a proper respirator fit test until OSHA showed up last month.” These stories highlight a critical gap: enforcement and culture.
An industrial hygienist on r/OccupationalMedicine noted: “The biggest challenge isn't the technology but getting workers to consistently wear P-100 respirators in 90+ degree heat on construction sites-compliance drops to 40% in summer months.” Discomfort leads to shortcuts. Shortcuts lead to disease.
The CDC’s NIOSH Health Hazard Evaluation Program found that 68% of worker complaints about respiratory protection were related to improper fit or discomfort. Thirty-two percent admitted modifying their respirators to make them more comfortable-compromising their own safety.
Health Monitoring: Catching Problems Early
You can’t feel early-stage lung damage. By the time you’re struggling to breathe, it’s often too late. That’s why health monitoring is crucial.
Work Health Solutions recommends spirometry testing at baseline and at least every five years for workers exposed to respiratory hazards. If you have pre-existing conditions like asthma, annual testing is advised. The American Thoracic Society emphasizes that early detection can slow disease progression by 30-50%.
Don’t wait for symptoms. Get tested. Keep records. Share results with your employer. You have the right to a healthy workplace-and the responsibility to protect yourself.
Building a Culture of Safety
Prevention isn’t just about rules. It’s about mindset. Successful programs require buy-in from everyone-from supervisors to entry-level workers.
A case study from Work-Fit documented 15 construction companies that reduced respiratory incidents by 65% over three years. Their secret? Supervisors modeled proper PPE use 100% of the time. Workers felt empowered to report unsafe conditions without fear of retaliation. Respirators were stored in clean containers. Fit testing happened annually-not just when inspectors visited.
OSHA’s Whistleblower Protection Program reinforces this: reporting hazards shouldn’t cost you your job. It should save your life.
What’s Next for Occupational Lung Disease Prevention?
Progress is being made. NIOSH launched its ‘Prevent eTool’ digital platform in 2023, providing industry-specific guidance for 15 high-risk sectors. Early data shows a 40% reduction in respiratory incidents among participating companies within six months.
OSHA’s National Emphasis Program on silica has conducted over 1,200 inspections since October 2022, resulting in nearly 1,000 citations. Average penalties hover around $3,125 per violation-a signal that regulators are serious.
The European Respiratory Society aims to eliminate occupational lung diseases by 2030 through coordinated action across 30 countries. Pilot programs in Germany already show a 55% reduction in new cases thanks to mandatory health surveillance and exposure monitoring.
New technologies like wearable sensors that provide real-time dust exposure data promise even greater precision. But tech alone won’t solve the problem. We need cultural shifts. We need leaders who prioritize health over speed. We need workers who speak up.
Can silicosis be cured?
No, silicosis cannot be cured. The scarring in the lungs is permanent. Treatment focuses on managing symptoms and slowing progression, but prevention is the only way to avoid the disease entirely.
How long does it take for asbestosis to develop?
Asbestosis typically develops 20 to 40 years after initial exposure. This long latency period means symptoms may not appear until decades after the last exposure, making early monitoring essential.
Is an N-95 mask enough to protect against silica dust?
An N-95 mask filters 95% of particles 0.3 microns in size, which offers some protection. However, for heavy silica exposure, higher-efficiency respirators like P-100 (99.97% filtration) are recommended, along with engineering controls like wet cutting and ventilation.
Who is at highest risk for occupational lung diseases?
Workers in construction, mining, manufacturing, shipbuilding, and demolition face the highest risk. Older workers (over 55) are also more vulnerable due to potential pre-existing respiratory conditions and cumulative exposure.
What should I do if I suspect asbestos in my workplace?
Do not disturb the material. Report it to your supervisor or safety officer immediately. Only certified professionals should handle testing and abatement. Never attempt DIY removal.
How often should I get spirometry testing if I’m exposed to silica or asbestos?
Baseline testing is required upon hiring. Follow-up tests should occur at least every five years, or annually if you have pre-existing respiratory conditions or high-level exposure.
Are there legal requirements for respirator fit testing?
Yes, under OSHA standard 1910.134, all employees required to wear respirators must undergo annual fit testing to ensure proper seal and effectiveness. Employers must also provide training and maintain records.
Can smoking worsen occupational lung disease?
Absolutely. Smoking increases the risk of developing occupational lung diseases by 50-70%, according to the American Lung Association. Combined exposure multiplies damage significantly.
Alexa Mack
May 3, 2026 AT 01:43