The First Line of Defense: Lifestyle Tweaks
Before reaching for the medicine cabinet, the first stage of management focuses on the physics of your body. Your Lower Esophageal Sphincter (or LES) is the valve that keeps acid down. When this valve is weak or under too much pressure, acid escapes upward. One of the most effective changes you can make is adjusting your sleeping position. Elevating the head of your bed by about six inches uses gravity to keep acid where it belongs while you sleep. Similarly, pay attention to when you eat. Lying down within an hour of a meal can increase reflux episodes by 50%. Try to stay upright for at least three hours after dinner before hitting the pillow. Weight management also plays a huge role. If you're overweight, losing just 10% of your body weight can lead to a 40% improvement in symptoms. This happens because excess abdominal fat puts physical pressure on the stomach, forcing acid through the LES. Additionally, quitting smoking is critical; nicotine relaxes the LES, reducing its pressure by as much as 30-40% within just twenty minutes of a cigarette.Eating for Relief: Identifying Your Triggers
Not all "trigger foods" affect everyone the same way, but some are notorious for causing chaos. High-fat meals are a major culprit, often delaying gastric emptying by up to an hour and increasing reflux episodes by 40%. If you want to see a real difference, try keeping your dietary fat intake below 30% of your total calories. Common offenders include:- Caffeinated drinks: Coffee and energy drinks can boost gastric acid production by 23% shortly after consumption.
- Mint and Chocolate: Peppermint relaxes the LES by up to 20%, while the methylxanthine in chocolate does something similar.
- Acidic foods: Citrus fruits (pH 2.0-4.0) and tomato-based products (pH 4.0-4.6) directly irritate the lining of the esophagus.
- Carbonation: Fizzy drinks cause gastric distension, which increases internal abdominal pressure by 15-20 mmHg.
Understanding Your Medication Options
When lifestyle changes aren't enough, we move into the medical stages of treatment. These range from quick fixes to long-term acid suppression.| Medication Type | Examples | How it Works | Speed of Relief | Duration |
|---|---|---|---|---|
| Antacids | Tums (Calcium Carbonate) | Neutralizes existing acid | Immediate | 30-60 Minutes |
| H2 Blockers | Pepcid (Famotidine) | Reduces acid production | Within 60 Mins | 10-12 Hours |
| PPIs | Nexium, Prilosec | Shuts down acid pumps | 1-4 Hours | 24 Hours |
| P-CABs | Voquezna (Vonoprazan) | Rapid, potent acid blocking | Very Fast | Sustained 24h |

The Newest Innovations and Long-Term Risks
While PPIs are effective, some people experience "nocturnal acid breakthrough," where acid returns at night. This is where Potassium-Competitive Acid Blockers (P-CABs), such as vonoprazan, come in. Approved recently by the FDA, P-CABs provide a more rapid and sustained acid suppression than traditional PPIs, with 95% of patients maintaining a healthy pH level for a full 24 hours. It is worth noting that long-term PPI use (over a year) isn't without risks. The FDA has highlighted potential issues including a higher risk of Clostridium difficile infections and chronic kidney disease. Some users also report magnesium or Vitamin B12 deficiencies. Because of this, it's a good idea to have your serum magnesium levels checked every six months if you've been on a PPI for a long time.When Surgery Becomes the Solution
For the 10-15% of patients who don't respond to meds or who simply don't want to take a pill every day for the rest of their lives, surgical intervention (Stage V) is an option. The traditional "gold standard" is Laparoscopic Nissen Fundoplication. This procedure wraps the top of the stomach around the LES to tighten the valve. It has a very high success rate-around 90-95%-but can sometimes lead to "gas-bloat syndrome," where you have trouble burping or vomiting. Another modern option is the LINX Reflux Management System. Instead of rearranging your stomach, a surgeon implants a small titanium bead bracelet around the LES. It keeps the valve closed to acid but opens for food. About 85% of patients stay off PPIs five years after this procedure, though it's not for everyone-specifically those who might need an MRI in the future or those who have had previous gastric surgery.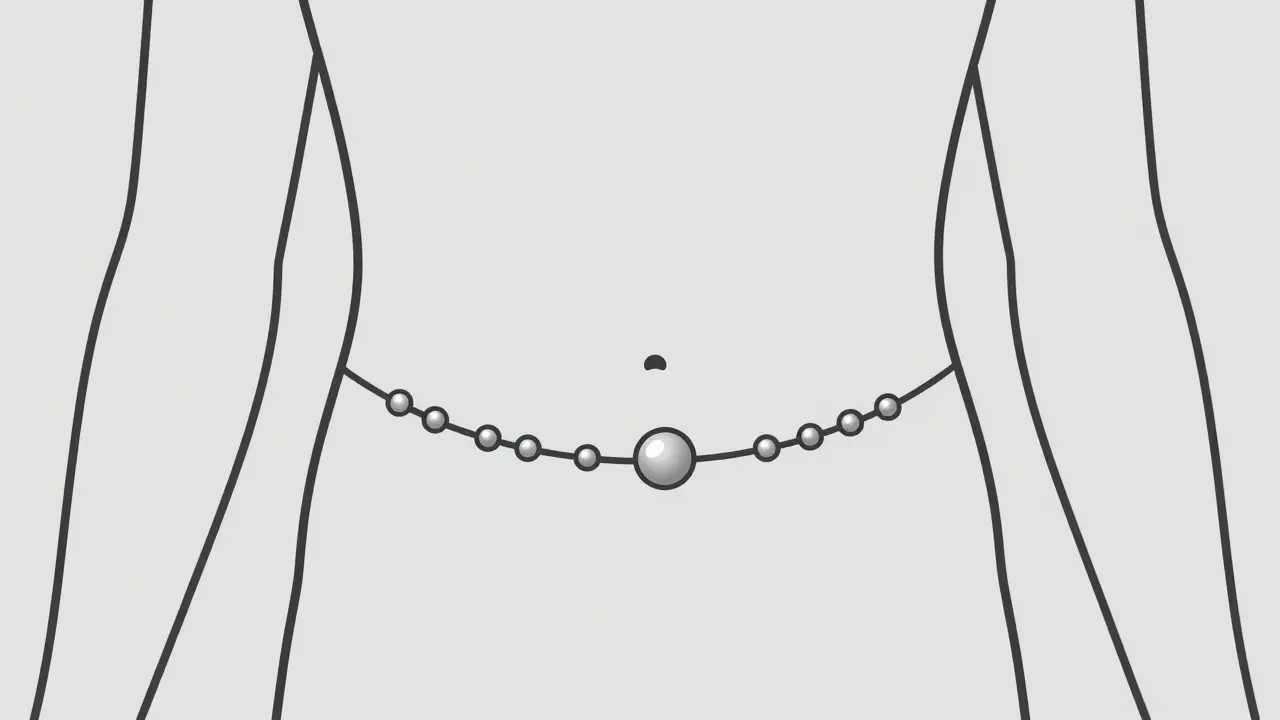
Practical Tips for Daily Maintenance
Managing GERD is often a game of consistency. Beyond the meds and diet, simple habits can make a massive difference. Diaphragmatic breathing-deep belly breathing-practiced for 15 minutes after meals has been shown to reduce symptoms in mild cases by 35%. If you're struggling to find a balance, remember that your treatment can evolve. You might start with a strict low-fat diet and bed elevation, move to an H2 blocker for occasional flare-ups, and only progress to PPIs or P-CABs if necessary. The key is to work with a provider to ensure you aren't over-medicating if lifestyle changes can do the heavy lifting.How long does it take for PPIs to start working?
While you might feel some relief within 1 to 4 hours, PPIs typically require 2 to 5 days of consistent daily dosing to reach their maximum acid-suppressing effect.
Can I completely cure GERD with diet alone?
For some people, yes. Those who successfully implement a strict low-fat diet (often under 20g of fat per day) and use head-of-bed elevation have reported eliminating symptoms without medication. However, this varies by individual and severity of the condition.
What is the difference between heartburn and GERD?
Heartburn is a symptom-the actual burning feeling. GERD is the chronic disease. If you have heartburn more than twice a week or it's causing damage to your esophagus, it's classified as GERD.
Are there side effects to taking PPIs for years?
Yes. Long-term use is associated with an increased risk of community-acquired pneumonia, C. diff infections, and kidney disease. There is also a risk of magnesium and Vitamin B12 deficiency.
Is the LINX device better than surgery?
It depends on your needs. The LINX device allows many to stop daily medications with a lower risk of gas-bloat than fundoplication, but it is contraindicated for patients who need MRIs or have had prior gastric surgeries.

Sam Hayes
April 4, 2026 AT 09:51