Imagine you're with a friend who has suddenly stopped responding. They're slumped over, their breathing is shallow or gone, and you can't wake them up no matter how hard you shout or shake them. In those seconds, the difference between a tragedy and a saved life comes down to one thing: knowing how to spot an opioid overdose and having naloxone is a life-saving medication that can rapidly reverse the effects of an opioid overdose on hand. When a person's brain is overwhelmed by opioids, the part that tells the body to breathe simply shuts down. Without intervention, brain damage starts in as little as four minutes. This guide is about the practical, immediate steps you need to take to stop a fatal overdose in its tracks.
Quick Guide to Saving a Life
- Spot the signs: Unresponsiveness, pinpoint pupils, and slow or absent breathing.
- Act fast: Call emergency services and administer naloxone immediately.
- Keep going: Perform rescue breathing and give a second dose of naloxone if there's no improvement after 2-3 minutes.
- Stay put: Never leave a person alone after they wake up; they may overdose again.
How to Spot an Opioid Overdose
Recognizing an overdose quickly is your first and most important job. Opioids-whether they are prescription painkillers or illicit drugs-hit the brain's respiratory center. When too much enters the system, the breathing rate often drops below 12 breaths per minute, and in severe cases, it stops entirely.
Look for these specific red flags:
- The "Unwakeable" State: The person won't respond to your voice or a firm sternal rub (rubbing your knuckles hard against their chest bone).
- Respiratory Distress: Breathing is very slow, irregular, or sounds like a "death rattle" (gurgling or snoring sounds). You might see only one breath every 3 to 5 seconds.
- Physical Discoloration: Check the lips and fingernails. In lighter skin tones, they may look blue or purple. In darker skin tones, look for an ashen or grayish cast. This is known as cyanosis.
- Pinpoint Pupils: The pupils of the eyes will be tiny, like the head of a pin, and won't react to light.
- Cold and Clammy Skin: The skin often feels damp and cold to the touch.
The Role of Fentanyl in Modern Overdoses
It's not just about heroin anymore. Fentanyl is a potent synthetic opioid that is 50 to 100 times stronger than morphine and is now found in a huge percentage of illicit drugs. Because it is so powerful, fentanyl overdoses happen much faster and often require more naloxone to reverse.
If you suspect fentanyl is involved, be prepared for a more stubborn reversal. While a single dose of naloxone might work for a lower-potency opioid, fentanyl often requires a second or third dose because it binds so strongly to the brain's receptors. If the person isn't breathing better after 2 or 3 minutes, don't hesitate to give another dose.
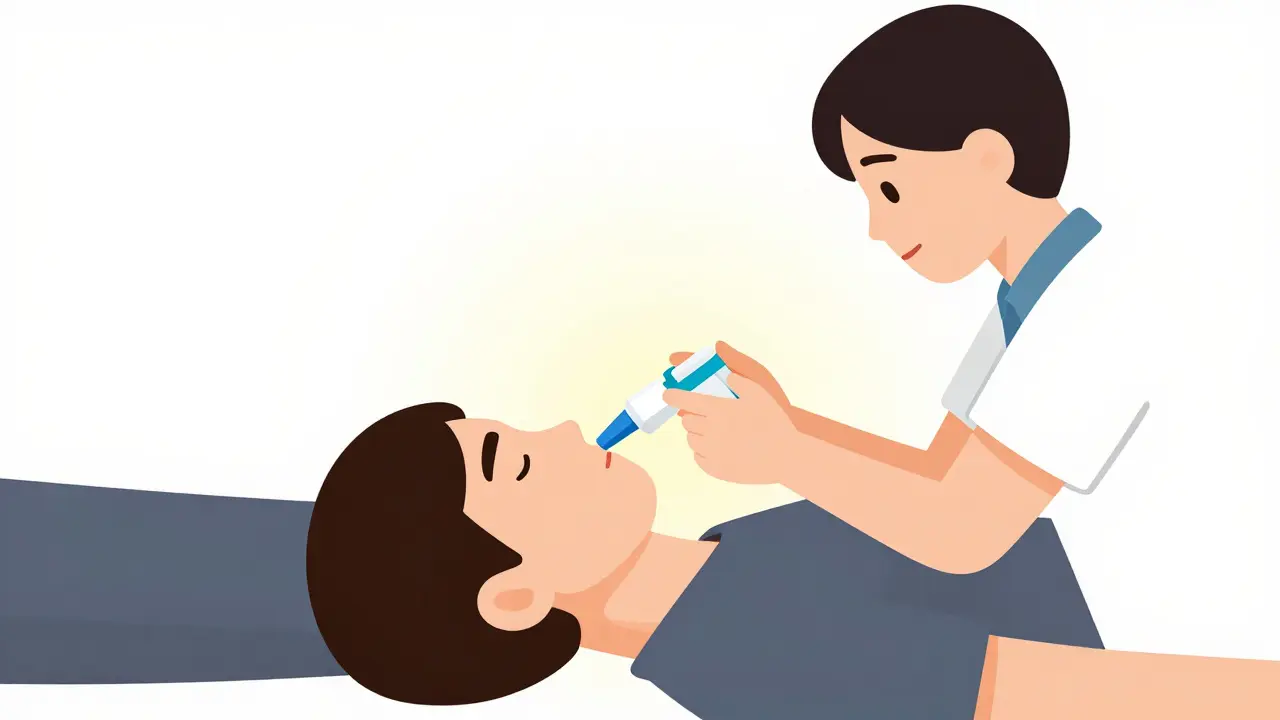
Step-by-Step: Using Naloxone to Reverse an Overdose
Naloxone works by acting like a "key" that kicks the opioid "lock" out of the brain's receptors, allowing the person to start breathing again. It doesn't matter if you aren't 100% sure it's an opioid overdose-naloxone will not harm someone who hasn't taken opioids, so it's always safer to use it if you're unsure.
Follow this protocol for the best chance of success:
- Check for Responsiveness: Shake them and shout. If there's no response, you have an emergency.
- Call 911 (or local emergency services): Do this immediately. Professional medical care is needed even if the person wakes up.
- Administer the Medication:
- Intranasal Spray (like Narcan): Gently insert the tip into a nostril and press the plunger.
- Intramuscular Injection: Inject the medication into a large muscle, such as the outer thigh.
- Provide Rescue Breathing: If they aren't breathing, tilt the head back, pinch the nose, and give mouth-to-mouth breaths. Aim for 10 to 12 breaths per minute, ensuring the chest rises with each breath.
- Wait and Repeat: Wait 2 to 3 minutes. If they haven't woken up or their breathing is still dangerously slow, administer a second dose.
| Formulation | Administration Method | Peak Effect Time | Best For... |
|---|---|---|---|
| Intranasal Spray | Nasal spray (no needle) | 5-10 minutes | Bystanders and quick deployment |
| Intramuscular (IM) | Injection into thigh/shoulder | 2-5 minutes | Faster onset of action |
| Auto-injector | Press-and-hold device | 2-5 minutes | Those afraid of needles |
Opioids vs. Stimulants: Knowing the Difference
It can be confusing when someone is unconscious, but it's vital to distinguish between an opioid overdose and a stimulant overdose (like cocaine or methamphetamine). These two scenarios are almost opposites in terms of physical symptoms.
While an opioid overdose causes the body to shut down (slow breathing, cold skin), a stimulant overdose-often called "overamping"-causes the body to accelerate. You'll see rapid breathing (over 24 breaths per minute), extremely high body temperature, agitation, and even seizures. In some cases, a stimulant overdose can lead to a stroke or heart attack, marked by chest pain or facial numbness.
What happens if they've taken both? This is called polysubstance use. The stimulants might mask the respiratory depression of the opioids, but as the stimulants wear off, the opioid overdose can suddenly hit. This is why naloxone is still the right move; it won't hurt a stimulant user, but it will save an opioid user.

Critical Mistakes to Avoid
When panic sets in, people often try "home remedies" that are actually dangerous. Here is what you should never do during an overdose:
- Don't put them in a cold bath: You might think you're "shocking" them awake, but you're actually risking drowning or inducing hypothermia.
- Don't inject them with salt water or other stimulants: Injecting coffee or other substances is ineffective and can cause severe infections or heart complications.
- Don't leave the scene: Naloxone is temporary. It typically lasts between 30 and 90 minutes. Many opioids, especially fentanyl, last much longer. Once the naloxone wears off, the opioids can re-attach to the receptors, and the person can slip back into an overdose.
- Don't forget the recovery position: If the person is breathing but unconscious, or if they start vomiting, roll them onto their side. This prevents them from choking on their own vomit (aspiration).
Getting Help and Legal Protections
A common fear is that calling for help will lead to arrest for drug possession. In many places, this is no longer a barrier. Good Samaritan laws are designed to protect people who seek emergency medical help for an overdose. These laws provide limited immunity from prosecution for drug possession to encourage bystanders to act without fear.
Naloxone is now widely available. In many regions, you can get it at a pharmacy without a prescription. It's also often distributed for free by community health centers and harm reduction programs. If you know someone at risk, having a kit in your bag or car is a simple way to potentially save a life.
Does naloxone work on all types of overdoses?
No. Naloxone only works on opioids (like heroin, oxycodone, and fentanyl). It will not reverse an overdose caused by alcohol, benzodiazepines (like Xanax), or stimulants (like cocaine). However, it is safe to administer if you aren't sure what the person took.
Will the person feel withdrawal symptoms after naloxone?
Yes. Because naloxone kicks the opioids off the brain receptors almost instantly, the person may wake up in "precipitated withdrawal." They might be confused, agitated, or feel sick. It's important to keep them calm and ensure they don't take more drugs to stop the withdrawal, as this could lead to another overdose.
How long does naloxone last in the body?
Naloxone typically lasts between 30 and 90 minutes. Many opioids remain in the system longer than that. This means a person can "re-overdose" after the naloxone wears off, which is why medical observation at a hospital is critical.
Can I use naloxone if the person is still breathing but barely?
Yes. You don't have to wait for them to stop breathing entirely. If they are unresponsive and their breathing is slow or shallow, administer naloxone immediately to prevent full respiratory arrest.
Where can I get naloxone without a prescription?
In many US states and Canadian provinces, pharmacies can dispense naloxone via standing orders. Community health clinics, syringe service programs, and some public libraries also provide free kits.

danny Gaming
April 13, 2026 AT 23:41