When a life-saving drug hits the market, the clock starts ticking. Twenty years after its original patent is filed, competitors can legally make the same medicine for a fraction of the cost. But what if that clock could be reset? That’s the reality of evergreening - a legal, but deeply controversial, strategy used by big pharmaceutical companies to stretch out monopoly control over drugs long after their original patents expire.
It’s not science fiction. It’s happening right now. Take Humira, the autoimmune drug that once generated $40 million a day in sales. AbbVie filed 247 patent applications around it. Over a decade, those patents stacked up like a wall, blocking generics from entering the market. The result? Patients paid thousands per month. When generics finally arrived in 2023, prices dropped by more than 80%. But by then, millions had already been overcharged.
How Evergreening Works: The Patent Game
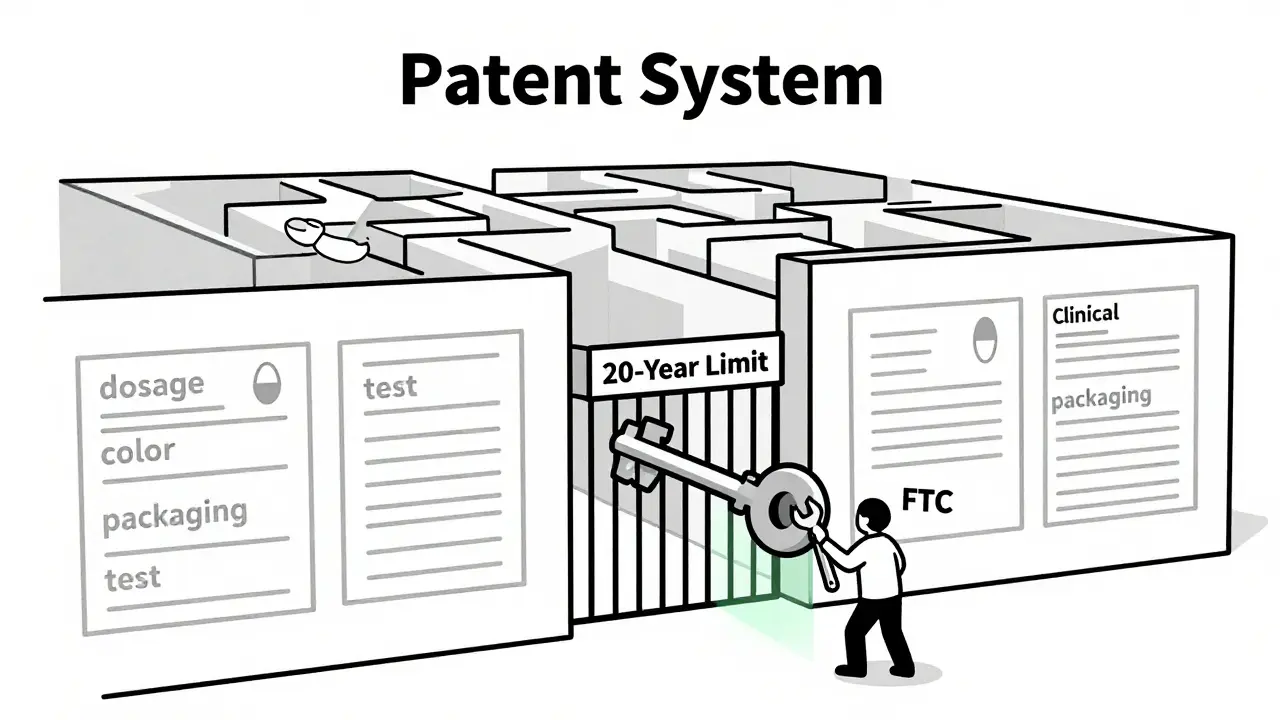
Every new drug gets a 20-year patent from the date it’s filed. That’s the legal limit. But evergreening doesn’t rely on inventing new drugs. It relies on making tiny changes - so small they often don’t improve how the drug works - and then filing a new patent for each one.
Here’s how it plays out in real life:
- A company makes a pill that works well. Patent expires in 2025.
- They change the coating to make it dissolve slower. New patent filed. Expiry pushed to 2030.
- They combine it with another drug already on the market. New patent. Expiry to 2033.
- They switch from a pill to an injection. New patent. Expiry to 2036.
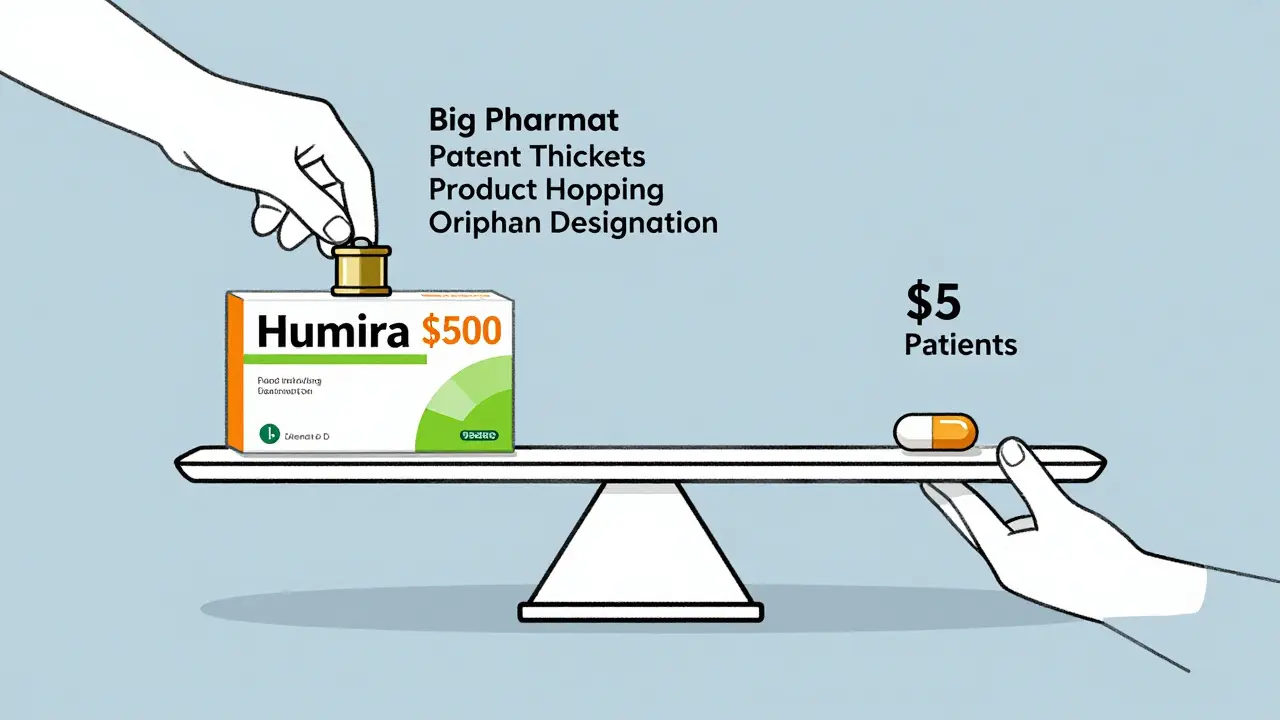
This isn’t innovation. This is patent stacking. Each tweak doesn’t make the drug better - it just delays the day when a $5 generic version can replace the $500 brand-name version.
The U.S. Hatch-Waxman Act of 1984 was meant to balance innovation and access. It gave brand-name companies a head start but promised generics a clear path in. But companies found loopholes. The law didn’t stop them from filing patent after patent for minor changes. Today, 78% of all new drug patents are for existing drugs - not new ones.
The Big Playbook: Tactics Used by Big Pharma
There’s no single way to evergreen a drug. There are dozens. Here are the most common ones:
- Product Hopping: This is when a company suddenly pulls an old version off the market and pushes a new one - even if it’s nearly identical. AstraZeneca did this with Prilosec (omeprazole) and Nexium (esomeprazole). Nexium was just a slightly modified version of Prilosec. But they marketed it as “better,” switched prescriptions, and kept sales high. The FDA approved it as a new drug. The patent clock reset.
- Orphan Drug Designation: If a drug treats a rare disease, it gets seven years of exclusivity. Some companies reclassify common conditions as “rare” in specific patient groups just to qualify.
- Pediatric Extensions: If a company tests a drug on children, they get six extra months of exclusivity. Many do this even when there’s no real clinical need.
- Authorized Generics: The brand-name company itself licenses a generic version to sell under a different name. It looks like competition, but it’s still their product. This keeps the market confused and delays true generic entry.
- Patent Thickets: Instead of one patent, companies file dozens - covering dosage, delivery method, packaging, manufacturing process, even the color of the pill. Generic makers can’t afford to fight them all in court.
AstraZeneca alone extended patent protection on six top drugs by more than 90 years combined. That’s not innovation. That’s financial engineering.
Why This Matters: Real People Pay the Price
Every time a patent is extended, patients pay more. Generic drugs typically cost 80-85% less than brand-name versions. That’s not a guess - it’s data from the FDA and independent studies. When generics enter, prices crash. When they’re blocked, prices stay high.
Consider diabetes drugs. Millions of Americans need insulin. One version, Lantus, had its patent extended multiple times. By the time generics arrived, many patients had skipped doses because they couldn’t afford it. The same story repeats with drugs for arthritis, depression, and high blood pressure.
It’s not just about money. It’s about health. A 2023 WHO report found that evergreening directly harms access in low- and middle-income countries. People there can’t wait years for a cheaper version. They die waiting.
Who’s Fighting Back?
Regulators are starting to push back. In 2022, the U.S. Federal Trade Commission sued AbbVie over Humira’s 247 patents, calling them “anticompetitive.” The case is still ongoing. The Inflation Reduction Act of 2022 gave Medicare the power to negotiate prices for the most expensive drugs - a direct hit to evergreening’s profit model.
The European Medicines Agency now requires proof of “significant clinical benefit” before granting extra exclusivity. That’s a big shift. No more patents for minor tweaks that don’t help patients.
But the system is still tilted. It takes years to challenge a single patent. Most generic companies don’t have the resources. And even when they win in court, the brand-name company just files another patent.
The Future: Biologics, Nanotech, and the Next Wave
Evergreening isn’t slowing down. It’s evolving.
Now, companies are moving to biologics - complex drugs made from living cells. These are harder to copy than chemical pills. A biologic generic (called a biosimilar) can take 10 years and hundreds of millions to develop. That gives companies more time to layer on new patents.
Some are even patenting genetic tests that predict how a patient will respond to a drug. If you need the test to use the drug, and the test is patented, you can’t use the generic - even if the drug itself is off-patent.
And then there’s nanotechnology. A drug that’s been around for 20 years? Coat it in nanoparticles. Patent the coating. Claim it’s a new delivery system. That’s already happening.
What’s next? Companies are testing “supragenerics” - their own generic versions sold under a different brand. It looks like competition. It’s not. It’s still the same company, same factory, same price.
Is There a Better Way?
Yes. And it’s simple: reward real innovation, not legal loopholes.
Developing a new drug costs $2.6 billion and takes 10-15 years. That’s expensive. But changing a pill’s coating? That costs $10 million and takes two years. Yet both get the same 20-year monopoly.
The system is broken. We’re paying billions for patents that don’t improve health. We’re delaying access to affordable medicine while companies chase profits.
What needs to change? Stricter rules on what counts as “inventive.” A cap on the number of patents per drug. Automatic generic entry if no clinical improvement is shown. And penalties for companies that use authorized generics to delay real competition.
The goal shouldn’t be to stop innovation. It should be to stop gaming the system.
Is evergreening illegal?
No, evergreening isn’t illegal - at least not yet. It’s a legal strategy that exploits gaps in patent law. Companies follow the rules, even if those rules let them extend monopolies with minor changes. Courts have sometimes blocked specific patents when they’re clearly obvious or not novel. But there’s no law that bans the practice as a whole. That’s why regulators are now pushing for reform.
How long can a drug’s exclusivity last with evergreening?
A drug’s original patent lasts 20 years from filing. But with evergreening, total exclusivity can stretch to 30, 40, or even more than 50 years. For example, AstraZeneca’s Nexium received multiple patent extensions, delaying generics for over 20 years beyond the original drug’s patent. In extreme cases like Humira, patent stacking pushed exclusivity past 30 years.
Do generics ever win against evergreening?
Yes, but it’s hard. Generic manufacturers have successfully challenged patents in court - especially when the modifications are clearly trivial. In 2023, Humira generics entered the U.S. market after years of legal battles. But each challenge costs millions. Many smaller generic companies can’t afford to fight. That’s why patent thickets work - they drown competitors in legal costs.
Does evergreening affect drug quality?
Not directly. The new versions are usually just as safe as the original. But they’re rarely better. The problem isn’t safety - it’s cost. Patients end up paying more for a drug that works the same way. In some cases, switching formulations causes side effects or requires new dosing, which can harm patients who are stable on the original version.
What’s being done to stop evergreening?
The U.S. FTC is suing companies like AbbVie. The Inflation Reduction Act lets Medicare negotiate prices, reducing the financial incentive to extend patents. The EU now requires proof of real clinical benefit. Some states are passing laws to block product hopping. And public pressure is growing. But without sweeping patent reform, companies will keep finding new ways to delay generics.
Every time a patent is extended, someone pays more for medicine they need. That’s not a side effect - it’s the point of the strategy. The question isn’t whether evergreening works. It’s whether we’re okay with paying for it.

Jimmy V
March 13, 2026 AT 23:13